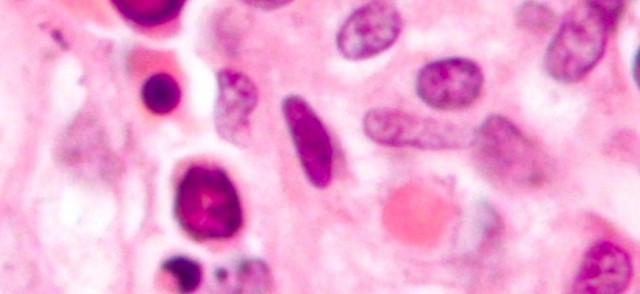
Tasty Morsels of EM 045 – Parvovirus B19
As always, this is from the ever expanding google doc on bits and bobs I read and learn from and transfer here for all our learning pleasure. Everyone knows the slapped cheek syndrome that runs in epidemics in kids. Hopefully … Read More »