I keep a little, ever-expanding note on my phone where I jot down little morsels of goodness that I pick up while listening to or reading one of the many excellent sites/podcasts in the useful resource section.
I’ll try and transfer them here for your enlightenment.
From this journal article:
SUTURE/STERI-STRIP COMBINATION FOR THE MANAGEMENT OF LACERATIONS IN THIN-SKINNED INDIVIDUALS The Journal of Emergency Medicine, Vol. 40, No. 3, pp. 322–323, 2011 PMID 20880653
Wounds on the skin of elderly folk on steroids are tough. Well they’re tough to fix at least. We all probably know that suturing is often not a good idea. But there are definitely places where you think a stitch or two would really help.
These guys suggest:
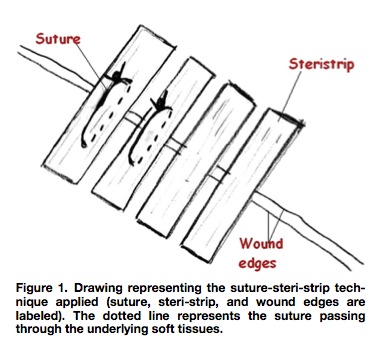
- Approximate the wound edges with steristrips as normal
- suture through the steristrips
From the paper:

Brill!!! Love it!! Thanks for posting. A tasty morsel indeed.
Pingback: The LITFL Review 025 - Life in the FastLane Medical Blog
is there an increase in infection rate as you are driving a foreign body, the steri strip , under the skin?
good question, not sure of the answer. though you shouldn’t really be driving the steri strip under the skin, it’s really there to provide an anchor for the suture. and anyhow the suture is the real foreign body here.
I use the horizontal mattress stitch in those thin skinned elbow flap lacerations. It does not tear and – if not overtightened (!!!) – it is very gentle on young and old skin alike, and does not leave cross hatching.
Cheers for the comment Peter, I suppose the key is in knowing when it’s too tight!
I agree that is the key – maybe why the Horiz Mattress is often avoided. Powerful tools need extra gentle hands.
With simple interrupted sutures, eversion and good dermal edge opposition is achieved only with good placement (e.g. flask/bottle shaped bites) and then only at the final tightening stage, but short of causing tissue ischaemia (or tearing).
Because the horiz mattress suture INHERENTLY everts, the window of eversion begins early. It goes against the grain, but IMHO, best to tie the HM only to the point where opposing edges meet (also bearing in mind the swelling which must also be accomodated during the first 48hrs of tissue inflammation during healing).
Building in some ‘slip’ into the knot is another safety feature possible – one double throw, one loose single throw, and then two+ tight single throws.
An afterthought is that the HM combines well with the steristrip trick, without having to pierce the strip.
Peter Ripley
I find that
1 ensuring that the wound is not oedematous (elevation, haemostatis /- compression
2 steristrips applied as a group of 5 ( the way the pack is designed). I usually cut the 1/8 inch in half to stop overlap on curved wounds
3 occassional use of wound glue to anchor the steristrips (either side of the wound)
is sufficient and has none of the issues associated with removing sutures and foreign body reaction.
None of this is successful without a non adherent compressive dressing, strict elevation (with DVT caution advice) for a period of 48 hours
I tell them
1 bed, bog, sofa
2 heel higher than knee, knee higher than hip
Remember what you are doing is a an autologous in situ split skin graft. As such it need the same level of love and attention.
Great tips thanks for that. Thinking of it as a skin graft is a great idea
Oh I could say a lot more about pretibials as its one of my faves.
1 All haematomas need evacuated
2 Entonox and grannies do mix (local doesnt)
3 Irrigation (tap water is fine) with a broken 21 guage needle hub and 20 ml syringe
4 Silver impregnated silicone dressing (you all know which one) for the ones that look a bit ropey
5 Never use viscopaste
6 Antibiotics rarely required
7 Practice model: a tomato that has a cut in it, dropped in boiling water for 30 secs: (best toy for this is a grapefruit segmenter punches tomato out like a pretibial flap)
Anybody got any other tricks
Crackin tips.
Do you evacuate pre-tib haematomas even when the skin is intact? I’ve seen a few disasters from that. Though to be fair the outcome may have been bad even if we didn’t do anything
Agree with the rest
Always.. Even if on warfarin
Just like on the scalp lacs … if you dont get the haematoma out… you dont get haemostasis.
For the shin the haematoma creates an impervious barrier to neovascularisation (necessary for the graft to take).
I incise on the most fleshy part (usually a paratibial medial incision X 1cm)
Its quite rewarding to evacuate the “blackcurrant jam” that lies beneath.
Using this technique on over 50 ladies (and 2 men) over the last number of years with complete success.
I do limit my interventions to wounds that are less than 48 hours old but prefer to be agressive on those that are less than 12 hours old. The others I “kick for touch” giving to plastics.
My regional plastics centre has more tnan 500 bed days for pretibial wounds annually. They wish that more ED docs were initially agressive.
BTW, the beauty of the steritrips technique is that it allows ooze to escape into the dressing.
Id be interested in others thoughts.
all right, you’ve convinced me, the next one i see gets a knife in the leg…
any papers to support it? I remember seeing one from plastics about it a year or so back but i can’t seem to find it on my computer
ya cant always get what you want…. as the Stones might say.
Talk to your plastics team… theres a multi-centre paper in it.
Ha! Fair enough!
I’ll ask mr/s plastic surgeon and the google.
Ive looked long and hard. Let me know what you find. One of the papers (from Wrexham I believe) was written by a staff grade who used to work in plastics… it was in EMJ a few years ago. I could’nt find much on the haematomas… I was just working from surgical first principles.