Ethics is tricksy.
No way round it.
There are lots of reasons for that, the type of thing that keeps philosophy and ethics departments in good work.
Approaches to ethics in med school are always going to be hopelessly inadequate, it’s perhaps unfair to expect much else.
This paper discusses ethics and how to train people in ethics in EM. And they say lots of good things. It’s just that it’s a tad reductionist for my liking.
Ethics curriculum for emergency medicine graduate medical education. J Emerg Med. 2011 May;40(5):550-6. Epub 2010 Oct 2. PMID 20888722
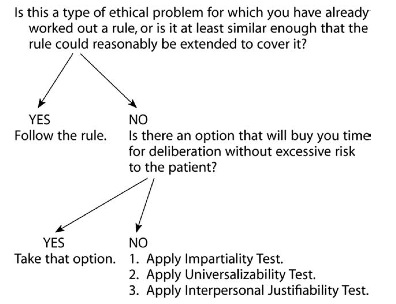
That figure may make a lot of sense to you. It certainly makes sense to me I’m just not sure it’s an entirely appropriate way to teach ethics or indeed practice it.
Or maybe it is. It’s probably a perfectly decent way to teach ethics if you believe that ethics is just another abstracted category to be put alongside physiology and anatomy.
The authors make this quote
a sound understanding of the principles of bioethics is necessary to become a compassionate and effective physician
Here I disagree. I do not know how an understanding of bioethics makes a doctor more or less compassionate.
Compassion in the context of virtue, character and humanity may be a learnable skill through the practice of a life lived but I’m not sure it’s teachable in the sense you can pass an MCQ at the end of it.
They do mention one thing that might be good material for fruitful reflection
Ethics education can be effectively provided, not only through behaviour modelling in the clinical environment, but also in formal didactic instruction
While I think the didactic instruction has its limitations as discussed above I think the “behaviour modelling” is fascinating.
Which brings me to this paper:
A Window on Professionalism in the Emergency Department Through Medical Student Narratives. Ann Emerg Med. 2011 May 28. [Epub ahead of print] PMID 21624702
Medicine is a lot like apprenticeship. In the sense that personalities and relationships are a key part of our learning and skill development. I model the behaviour and knowledge and skills that I find in my seniors.
These guys called the modelled professionalism by seniors “the hidden curriculum” which is kind of a neat name. Basically the students take on the habits of the seniors and the practices observed.
I am deeply grateful to the people I have worked with both for the things that they have taught me to do and the things that I have seen them do and vowed never to repeat!
The term “holistic” is in vogue when it comes to talking about patients. It’s unfortunate that it’s become a buzzword as it’s actually a useful reminder that we treat people, not just patients, and certainly not conditions.
To think of ethics training and the practice of medicine as easily definable and teachable components that can be formed in an algorithm is something I find quite inadequate.
Some (tongue in cheek) conflicts of interest:
- I think medical training is there to produce people capable of caring for the suffering, sick and the dying. These people need to both retain their own humanity and help their patients retain theirs. (This need not be in conflict with the good science and practices that fill medical research journals)
- As background to this I am not a materialistic determinist. I have problems with a lot of the assumptions modernity has given us. I am a confessing Christian and a big fan of virute ethics. Though I’ll gladly admit Aristotle was a bit bonkers on a whole range of things…
- I’m starting a masters in theology in the hope of exploring this kind of thing a bit further. And hopefully make it in some way intelligible and not just vague allusions to Macintyre…

Though it appears to be an oversimplification of sorts, this kmight just be the approach needed to drill the tricksy bits of ethics into our psyche as early as med student days. It is my personal experience that the traditional way of teaching ethics falls on deaf (and dead bored ears) when it comes to my country.
Cheers pranab
I suspect it’s an over simplification because I’m really only starting to think about this kind of thing!
Hmmm – I am somewhat in agreement with your take on this Andy. But for me there is just one important distinction in any discussion on this topic. There is a tendency in many people, articles and textbooks to consider ethics and morality to be the SAME THING.
I think ethics CAN be taught as a “subject” (albeit with varying theories or doctrines – somewhat akin to philosophy or theology, I guess) and can be practiced with varying degrees of compassion, but what cannot be taught is morality! Just to complicate things, morality is largely subjective – it is possible to have a correct “answer” to some ethical issues, but morality is in the eye of the beholder!
Semantics? – maybe, but ethics and morality are not synonymous!
Cheers for the comment domhnall
Really good point about morality and ethics being distinct that had me and a few mates debating it all morning!
There seemed two points in our discussion
– ethics is a technical description of morality, both it’s practice and methods
– morality informs ethics and vice versa in a kind of circularity that makes them seem synonomous
Not sure I’ve quite come down on which one yet!
Morality is a fairly dirty word these days it seems, and I in no way mean to dictate a very particular form of morality.
I am convinced that we are all moral people (doctors tend to be compassionate decent people) and are engaged in moral practices (like health care) and I think it’s useful to reflect upon ourselves as professional and a moral polis
God that sounds like a wordy sentence of mumbo jumbo…
Anyhow I’m still working a lot of this stuff out so forgive my inarticulate ramblings!
Always happy to stick my oar in and stir up some debate! I agree the two terms are deeply interlinked, and I agree we are (mostly, with some notable exceptions) moral people…BUT – we all have a different set of values shaping our morality which are very personal and shaped by many factors such as faith, upbringing, experience etc. In contrast, ethics, although there are different interpretations and theories, should be a relatively stable beast once one accepts the concept that what we do is for the good of the patient(s). There should be a certain reproducibility in ethics regardless of one’s moral standpoint, I think. But hey, I am no academic on this! What do I know!
Agree totally especially about the way our sense of morality is formed
Modern medical ethics has lots of value and as you say provides a consitency that may well be lacking otherwise. My thought Is more that it’s somewhat deficient description of what we do, not useless or wrong.
Pingback: Teaching is more important than research – discuss… | Emergency Medicine Ireland