 In Edinburgh they were changing to a more sensitive trop so they spent a few months using both but not telling the docs about the new cut-off. They then introduced it and looked to see if outcomes were different
In Edinburgh they were changing to a more sensitive trop so they spent a few months using both but not telling the docs about the new cut-off. They then introduced it and looked to see if outcomes were different
Patients
Included were all patients admitted to the hospital with suspicion of ACS.
Interventions
For the first few months every trop sent to the lab was done on the new more sensitive troponin but results were reported according to the old cut-off. The new, intermediate rage was recorded for the study but not reported to the docs. This was the validation phase.
For the next few months the new results were reported; the docs now knew that their patient had a trop between 0.05 and 0.02. Previously this would have been a -ve trop. This was the implementation phase.
Clear so far?
Results
The overall rule in rate (in terms of +ve trops) was 35% which is pretty high. I hear figures of 10% are more usual over in the US.
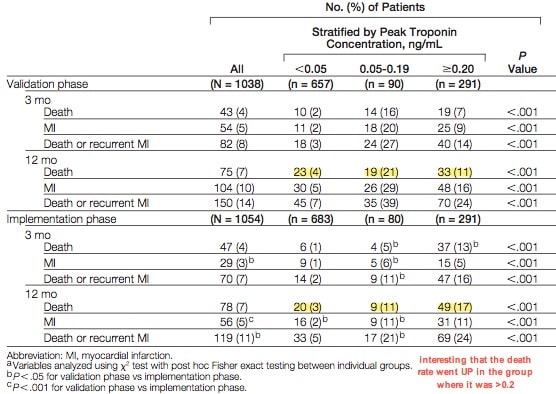
As expected, the new more sensitive troponin, with a lower cut-off, increased the diagnosis of MI dramatically. A +ve troponin being a key part of the diagnosis of MI.
But more interestingly are the clinical outcomes.
there was a 10% fall in death rate in people who would have previously ruled out with the old troponin. In other words people who were picked up in the new intermediate range (o.o5-0.2) had an absolute reduction in mortality of 10%.
That’s pretty powerful but the weird thing is that the death rate in the group who previously ruled in with the old trop went up about 8% when they introduced the new trop! Even though the trop range they fell into shouldn’t have been affected
It’s not totally fair to say it helped one group if it killed another (and not mention it; they just say that death and MI together were the same at 12 months!)
Also interesting that the patients who “needed” and apparently benefitted from the new trop were about 8 years older than the others. Understandably they did worse and had a higher mortality over all.
Comment
The methodology in this trial is pretty neat, providing a pretty nice control group for comparison. The fact that they measured clinical outcomes and not just diagnosis of MI means they care about the important outcomes.
The results (with both +ve and -ve changes in outcomes) might imply that there’s a base-line imbalance in the groups that predicts the mortality changes before and after.
Also worth noting that lots of +ve troponins aren’t anything to do with ACS, but are coming from PE, heart failure or sepsis. This might explain the peak of intermediate troponins in the elderly patients.
Please leave thoughts, comments or corrections below.