[If you want to hear the best thing I’ve heard on this yet then listen to the SMART EM podcast]
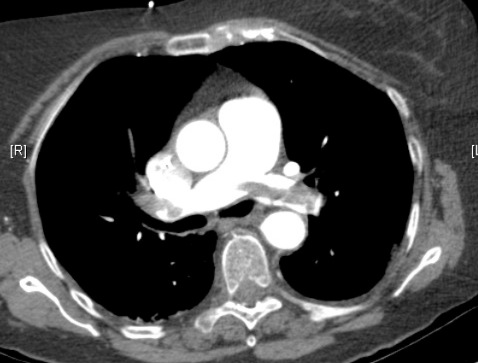 Perhaps I overstate things in the title, but I’m getting a little bit jaded with all things VTE these days.
Perhaps I overstate things in the title, but I’m getting a little bit jaded with all things VTE these days.
We were born and raised with the idea that PE carries with it a mortality rate of over 20% and that it’s this silent killer that’s knocking off patients left right and centre. And most importantly we’re missing it every day and all these people are dying because of it.
Does that sound familiar enough?
The past 15 years has seen the literature riddled with studies on VTE, largely diagnostic studies.
We are now picking up far greater numbers of VTE than ever before. We’re actually not bad it. It’s just a diagnosis of PE today is very different from diagnosis of PE say in 1960.
It seems pretty obvious that if our diagnostic models change then there’s a fair chance we’re diagnosing a different disease than we were 50 years ago.
The increased numbers we’re working up for PE, plus the increased sensitivity of the tests means we’re picking up smaller and smaller PEs.
But do we really think that a sub-segmental PE with minimal symptoms is the same beast as a saddle embolus with right heart failure?
Then why the hell are we still giving the same treatment to both!!!
We’re kind of getting into an evidence free zone. When it comes to treatment that is.
The evidence (as opposed to theory and observation) for anti-coagulation is mainly from here. An article cited 80 times has made some impact on the literature.
As described in the podcast above, this (non-randomised, non-blinded, no placebo) trial had 35 patients with PE diagnosed on clinical grounds only, not even a V/Q or an angio! Some got anti-coagulation, some got nothing.
After 35 were enrolled, 5 had died in the no anti-coagulation group and no one had died in the anti-coagulation group so they stopped the trial. Autopsies were done confirming largely massive PEs.
This is it. This is the foundation of our evidence for anti0coagulation in PE.
So our evidence for treatment is dodgy. Our evidence for treating sub-segmental PEs with minimal symptoms in otherwise low-risk patients is non-existent as far as I am aware. Please correct me if there’s stuff out there.
So what do I suggest?
Well something that is already being done – the risk-stratification of PE once the diagnosis is made. A lot of this is aimed at the massive and sub-massive PE patients, for whom tPA is probably a decent idea.
I suggest going a little further and using the new risk-stratification tools to find a population of people with small, sub-segmental PEs and low-risk for recurrence and not treat them with anything.
We’re already treating PE as an out-patient diagnosis and I suspect the reason they’re doing well is not because of the warfarin we give them but simply because they were going to do just fine anyhow.
Any thoughts?

Pingback: The LITFL Review 020 - Life in the FastLane Medical Blog
Pingback: Emergency Medicine Ireland - Life in the FastLane Medical Blog
Pingback: Outpatient versus inpatient treatment for patients with acute pulmonary embolism: an international, open-label, randomised, non-inferiority trial Lancet 2011; 378: 41–48 | Emergency Medicine Ireland
David missed the newly published article in Chest 2010; probably the most important article to be published on the topic. Take a look and let me know what you think. http://dl.dropbox.com/u/220032/peevidence.zip
cheers for that Scott. Will have a read and let you know my thoughts. I feel it might end up as a post on its own!
I’ve been reading through the Aujesky stuff too so it might get thrown in there too.
Actually autopsies were performed in all patients who died during the Barritt Jordan study. PE appeared to be the leading cause of death in the untreated group, and it seems likely since they all were overway massive PEs with huge lung infarctions. I think the title of the paper should have been “anticoagulation for massive PEs waiting for thrombolitic therapy to come”. Methodological flaws are all there. The authors were too confident with their conclusions, yet it was a different era. What strikes the most is the distorted use of the study results that was made over years. Passive acceptance of informations is the essence of dogma, but it’s probably the unavoidable starting point of every learning process. Great blog I keep reading it. I may send you a PDF in case you are still looking for this old but honorable publication.
Cheers for the comment Mattia
You’re right of course about the autopsies. I’ve since got a copy of the paper and managed to read it I just haven’t updated the post! (I have as of today.)
I like your alternate title for the paper, it would have been more accurate!
what was the paper quote here ?
“David missed the newly published article in Chest 2010; probably the most important article to be published on the topic. Take a look and let me know what you think. http://dl.dropbox.com/u/220032/peevidence.zip”
The dropbox link is outdated.